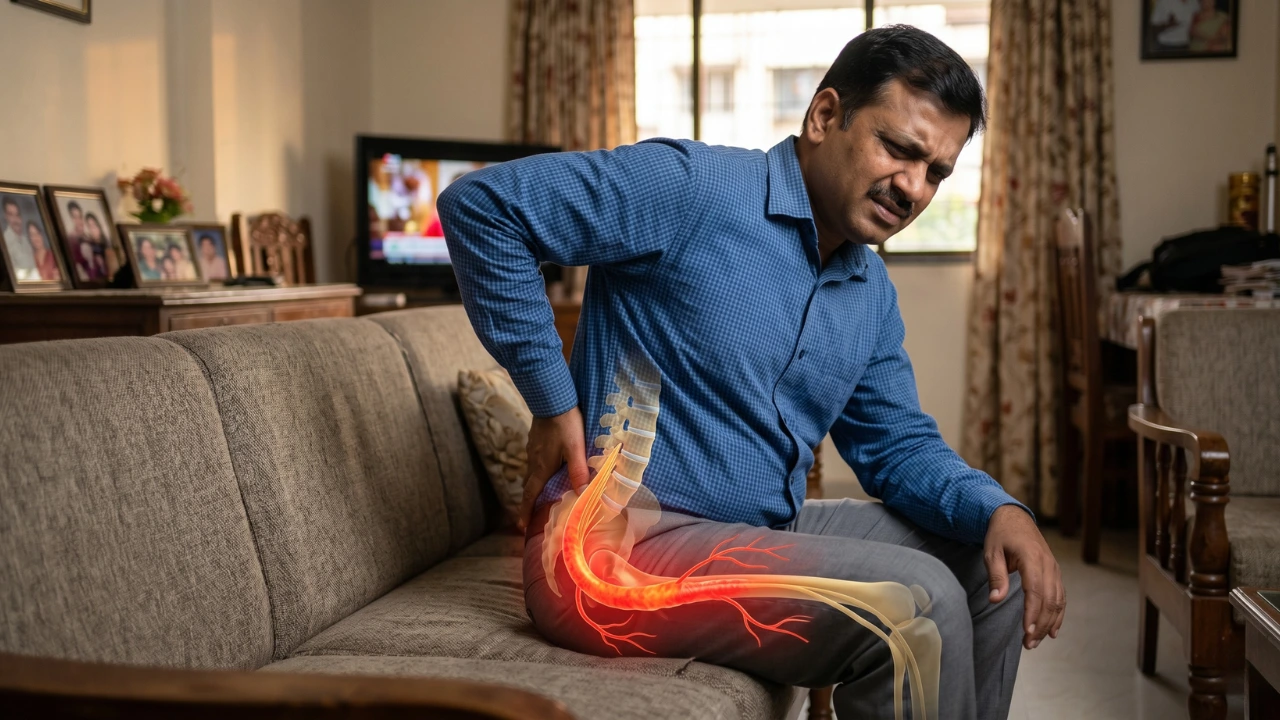
You felt it first as a dull ache in your lower back. Then one morning — maybe getting out of bed, or leaning forward to pick something up — a lightning bolt of pain shot from your lower back, through your buttock, and down your leg. Maybe it reached your calf. Maybe all the way to your foot.
You searched online. You found two words: sciatica and slip disc. You weren't sure which one applied to you. So you took a painkiller, told yourself it would pass, and waited.
That was three weeks ago.
If that story sounds familiar, please read every word of this article. Because the difference between sciatica and a slip disc is not just academic — it determines your diagnosis, your treatment, and whether you fully recover or spend the next year managing a condition that has quietly progressed while you waited.
The clinical team at Curis 360 Physiotherapy, Jayanagar — led by Dr. Ponkhi Sharma PT (19 years of experience) — sees this confusion every week. People who have spent months on the wrong treatment, or no treatment at all, because nobody took the time to properly explain what is actually happening inside their spine.
This article will.
First, the Most Important Fact Most People Don't Know
A slip disc and sciatica are not the same thing. But a slip disc can cause sciatica.
This is the relationship that confuses almost everyone:
- A slip disc (herniated or prolapsed intervertebral disc) is a structural injury to the disc between your vertebrae
- Sciatica is a set of symptoms — shooting leg pain, numbness, tingling — caused by compression or irritation of the sciatic nerve
- A slip disc pressing on the sciatic nerve root is the most common cause of sciatica (about 85% of cases)
- But sciatica can also be caused by other conditions — tight piriformis muscle, spinal stenosis, or sacroiliac joint dysfunction — with no disc involvement at all
This means: treating sciatica without knowing if there's a slip disc is like treating a fever without knowing the infection. The symptoms overlap enough to be confusing, but the treatment protocols are fundamentally different.
What Is a Slip Disc? (And Why "Slip" Is the Wrong Word)
The term "slip disc" is a misnomer that has persisted because it's easy to say. Discs don't actually slip — they herniate, bulge, or prolapse.
Between each pair of vertebrae in your spine sits an intervertebral disc: a shock-absorbing structure with a tough outer ring (the annulus fibrosus) and a soft, jelly-like centre (the nucleus pulposus). Think of it like a jam doughnut.
When the outer ring is weakened — by years of poor posture, repetitive bending, sudden loading, or natural degeneration — the inner material can push through and bulge outward. When it pushes far enough to press on an adjacent nerve root, that's when you feel it as leg pain.
The most commonly herniated levels in the lower back:
- L4–L5 disc → Pressing on the L4 or L5 nerve root → Pain down the outer calf and top of foot, sometimes with weakness when lifting the foot (foot drop in severe cases)
- L5–S1 disc → Pressing on the S1 nerve root → Pain down the back of the calf to the heel and outer foot, with reduced Achilles reflex in severe cases
Signs that point specifically to a slip disc:
- Pain that is worse when bending forward (flexion loads the disc, increasing herniation)
- Pain that improves slightly when walking or standing upright
- Pain that worsens dramatically with coughing, sneezing, or straining on the toilet (the Valsalva manoeuvre increases spinal canal pressure)
- A clear onset event — "I bent to pick something up and felt a sharp pop"
- Pain that is worse sitting for prolonged periods (disc pressure increases 40% when seated)
- Leg pain that is more intense than the back pain — this is a red flag for nerve root involvement
What Is Sciatica, Precisely?
Sciatica describes a specific pattern of symptoms — not a single cause. The sciatic nerve is the longest and widest nerve in the human body. It originates from nerve roots L4, L5, S1, S2, and S3 in your lumbar spine, travels through the buttock, down the back of the thigh, and branches into the lower leg and foot.
When this nerve is compressed, inflamed, or irritated anywhere along its path, you experience the classic sciatic distribution: shooting, burning, or electric pain from the lower back through the buttock and down the leg, often accompanied by tingling, numbness, or weakness.
Signs that point specifically to sciatica (without a disc cause):
Piriformis Syndrome:
- Pain deep in the buttock that worsens when sitting on hard surfaces
- Worsens with hip rotation — particularly when crossing your legs
- No pain with forward bending
- MRI of the spine is typically normal — but the sciatic nerve is being compressed by the piriformis muscle in the buttock
- Common in runners, cyclists, and people with one leg slightly shorter than the other
Lumbar Spinal Stenosis:
- Bilateral (both legs) heaviness or aching that comes on with walking or prolonged standing
- Relieves almost completely with sitting or leaning forward
- Age > 55 years (usually — but not always)
- Symptoms develop gradually over months to years
Sacroiliac (SI) Joint Referral:
- Pain concentrated around the sacroiliac joint (just lateral to the spine at the very bottom)
- Refers pain into the buttock and upper thigh, but rarely below the knee
- Aggravated by stair climbing, rolling over in bed, and single-leg activities
The Danger of Getting This Wrong
Here is what the clinical team at Curis 360 Jayanagar sees regularly — and it is, frankly, heartbreaking.
A patient comes in with six months of leg pain. They were told it was "just sciatica" and given a standard set of generic back exercises. But the exercises prescribed for piriformis syndrome are contraindicated for an acute disc herniation. Repeated forward bending — commonly prescribed for piriformis — can push a herniated disc further onto the nerve root.
Or the opposite: a patient with piriformis syndrome is put on bed rest and told to avoid all movement. The nerve becomes increasingly sensitised, the piriformis gets tighter from inactivity, and three months later the pain is far worse.
Every week delayed is a week of nerve irritation building scar tissue and sensitisation around the nerve. What could be resolved in 6 sessions at 6 weeks becomes 20 sessions at 6 months.
The Honest Question You Need to Ask Yourself
How long have you had this pain?
If the answer is more than two weeks — you have already waited longer than you should have. If the answer is more than a month — the disc, if involved, has been pressing on that nerve root for four weeks. Nerve roots under prolonged compression develop chronic inflammation that is far harder to resolve than acute compression.
And if the answer is "months" — there is something important you should know.
Most people who come to Curis 360 Jayanagar with chronic sciatica or slip disc say the same thing in their first appointment: "I kept thinking it would go away on its own."
Some of them are right. A small percentage of disc herniations do reabsorb over time with rest. But the majority do not. And for every week you wait, the muscles that support your lumbar spine are weakening, the nerve is becoming more sensitised, and the compensation patterns your body develops to avoid pain are causing secondary problems in your hip, opposite knee, and thoracic spine.
You know this. That quiet voice in the back of your mind that keeps saying "I really should get this checked" — that voice is right.
5 Symptoms That Mean You Need a Physiotherapy Assessment Today — Not Next Week
-
Leg pain that is worse than your back pain — This is the strongest indicator of nerve root involvement, whether disc or otherwise.
-
Numbness or tingling anywhere in your leg, calf, or foot — Altered sensation indicates nerve compression, not just muscle pain. This needs assessment before it progresses to weakness.
-
Weakness in the foot or ankle — Difficulty lifting the foot (foot drop), reduced push-off when walking, or inability to stand on tiptoe all indicate significant nerve compromise. Do not wait.
-
Pain that woke you from sleep — Sleep-disturbing pain typically indicates significant inflammatory activity or, in rare cases, a more serious underlying cause that needs to be ruled out.
-
Pain that has been present for more than 2 weeks without any improvement — Acute disc herniations typically improve noticeably within 10–14 days with appropriate management. If yours is not, you are likely not doing the right things.
One more, and this is urgent: If you have any loss of bladder or bowel control alongside your leg pain — this is a medical emergency called cauda equina syndrome. Go to the emergency department immediately. This is the only sciatica scenario that requires urgent surgery.
How Physiotherapy Differentiates and Treats Both Conditions
At Curis 360 Jayanagar, the first appointment for any patient with leg pain is a 45–60 minute clinical assessment — not a 10-minute consultation followed by generic exercises. The assessment includes:
Neurological examination:
- Dermatomal pain mapping (which nerve root is affected)
- Muscle strength testing (quadriceps, tibialis anterior, gastrocnemius, EHL)
- Reflex testing (patellar, Achilles)
- Sensation testing (light touch and pin-prick in leg dermatomes)
Orthopaedic tests:
- Straight Leg Raise (SLR) — a positive test at less than 45° strongly suggests disc herniation with nerve root compression
- Slump test — even more sensitive than SLR for disc-related sciatica
- FABER/FADIR tests — identifies sacroiliac or hip involvement
- Piriformis provocation tests — identifies piriformis syndrome
- Lumbar quadrant test — identifies facet joint or stenotic involvement
Directional preference assessment (McKenzie MDT): We identify whether repeated lumbar extension, flexion, or lateral movements cause your leg pain to "centralise" (move from the leg back into the back). This is one of the most powerful diagnostic and therapeutic tools available for disc-related sciatica — and it is only possible with a proper clinical assessment.
Treatment: Disc Herniation with Sciatica
- McKenzie Extension Protocol — The most evidence-based intervention for disc-related sciatica. Repeated extension movements encourage the disc material to migrate away from the nerve root, causing pain centralisation. Most patients with disc-related sciatica experience significant relief within 3–6 sessions.
- Neural mobilisation (nerve flossing) — Gently mobilises the sciatic nerve along its length, reducing adhesions and neural sensitisation
- Lumbar traction — Manual or mechanical decompression of the disc-nerve interface
- IFT (Interferential Therapy) — Deep electrical stimulation to reduce nerve root inflammation
- Progressive core stabilisation — Once acute pain is controlled, rebuilding the deep stabilisers (transversus abdominis, multifidus) that protect the disc
Treatment: Piriformis Syndrome
- Piriformis soft tissue release — Direct manual therapy to the piriformis muscle in the deep buttock, releasing the compression on the sciatic nerve
- Hip external rotator stretching programme — Sustained stretching of the piriformis and short external rotators
- Sciatic nerve mobilisation (neural flossing)
- Hip abductor and gluteal strengthening — Corrects the biomechanical causes of piriformis tightness
- Gait retraining — Corrects internal hip rotation and other gait faults that load the piriformis
At Curis 360 Jayanagar, we have seen patients with piriformis syndrome resolve completely in 4–6 sessions — patients who had previously been treated for 6 months for "disc problems" without improvement, because the diagnosis was simply wrong.
What Happens If You Keep Waiting
We want to be honest with you, because you deserve honesty.
If you have had leg pain for more than 4 weeks:
- The sciatic nerve has been under sustained compression or irritation
- Central sensitisation — where the nervous system amplifies pain signals — begins to develop
- The surrounding muscles are either weakening (disuse) or overactivating (guarding)
- The disc, if involved, is not healing as effectively without appropriate movement
If you have had leg pain for more than 3 months:
- You now have chronic sciatica — a fundamentally different clinical entity that requires more sessions, longer treatment, and carries a higher risk of incomplete resolution
- The probability that surgery will be recommended to you increases significantly, even though many of these patients could have been helped with proper physiotherapy at an earlier stage
The thing is — you probably already know this. The fact that you are reading this article tells us that your symptoms have been there long enough to push you toward looking for answers.
The answer is not another article. It is an assessment.
What Recovery Looks Like at Curis 360 Jayanagar
When patients from 7th Block, JP Nagar, BTM Layout, Koramangala, and across South Bangalore come to Curis 360 Jayanagar, this is what they experience:
Week 1–2: Accurate diagnosis. Pain begins to centralise (move from leg to back). Night pain reduces. The relief of finally knowing what is wrong is itself significant.
Week 3–6: Leg pain reduces substantially. Neural tension reduces. Daily activities become manageable again. Core rehabilitation begins.
Week 6–12: Most acute disc cases are at 70–85% recovery. Piriformis cases are often fully resolved. Return to normal daily activities and light exercise.
Week 12+: Full return to sport, gym, and occupational activities with a structured maintenance programme to prevent recurrence.
"I had shooting pain down my leg for four months before I came to Curis 360 Jayanagar. My orthopaedic surgeon had recommended surgery. After 8 sessions with Dr. Ponkhi's team, the leg pain was gone. I never needed surgery. I just needed the right physiotherapy." — Anand V., JP Nagar
Frequently Asked Questions
Can sciatica go away on its own without physiotherapy? In mild cases — particularly acute disc herniations in younger patients — some improvement can occur with rest alone. However, without treating the underlying cause (disc mechanics, piriformis dysfunction, core weakness), recurrence rates are extremely high. Physiotherapy significantly accelerates recovery and reduces recurrence by 60–70%.
Should I get an MRI before coming to physiotherapy? An MRI is not necessary before your first physiotherapy appointment. Our clinical assessment identifies the probable diagnosis and treatment direction from day one. If the MRI is relevant (e.g., to rule out serious pathology or guide treatment decisions), we will recommend it. Most acute sciatica cases do not need an MRI in the first 6–8 weeks.
How long does sciatica physiotherapy take at Curis 360 Jayanagar? Acute disc-related sciatica presenting within 4 weeks typically resolves in 6–10 sessions over 6–8 weeks. Piriformis syndrome resolves in 4–8 sessions. Chronic sciatica (3+ months) typically requires 12–20 sessions over 3–5 months.
Is it safe to exercise with a slip disc? Yes — with guidance. The wrong exercises worsen a disc herniation. The right exercises (identified through directional preference assessment) actively decompress the disc. This is why a physiotherapy assessment before starting any exercise is essential.
Can I come to Curis 360 Jayanagar even if I'm in a lot of pain? Absolutely. Our physiotherapists are trained to manage patients in acute, severe pain. We can treat you in the most comfortable position possible and design an initial programme that does not worsen your symptoms. Many of our most dramatic recoveries started with a patient who could barely walk into the clinic.
Book Your Assessment at Curis 360 Jayanagar — Before This Gets Worse
Curis 360 Physiotherapy — Jayanagar is Bengaluru's specialist physiotherapy clinic for sciatica, slip disc, and leg pain — directed by Dr. Ponkhi Sharma PT, with 19 years and over 5,000 patients of clinical experience.
We are located at 7th Block, Jayanagar, KR Road, Bengaluru — 10 minutes from JP Nagar, BTM Layout, Koramangala, and Banashankari.
- Sessions from ₹650
- No referral needed
- Monday–Saturday: 8:00 AM–8:30 PM
- Same-week appointments available
Book your sciatica assessment today or call +91 78998 44360.
Don't let another week of nerve compression become another month of chronic pain. The longer the nerve is irritated, the longer it takes to settle. But it can settle — with the right diagnosis and the right treatment. That's what we do, every day, at Curis 360 Jayanagar.

Dr. Ponkhi Sharma PT
Clinical Director at Curis 360. Specializing in advanced rehabilitation, evidence-based manual therapy, and holistic patient care in Bengaluru.
View Full Clinical Profile